Contact tracing, isolation, exposure lists: The things an 80% vaccination level will change

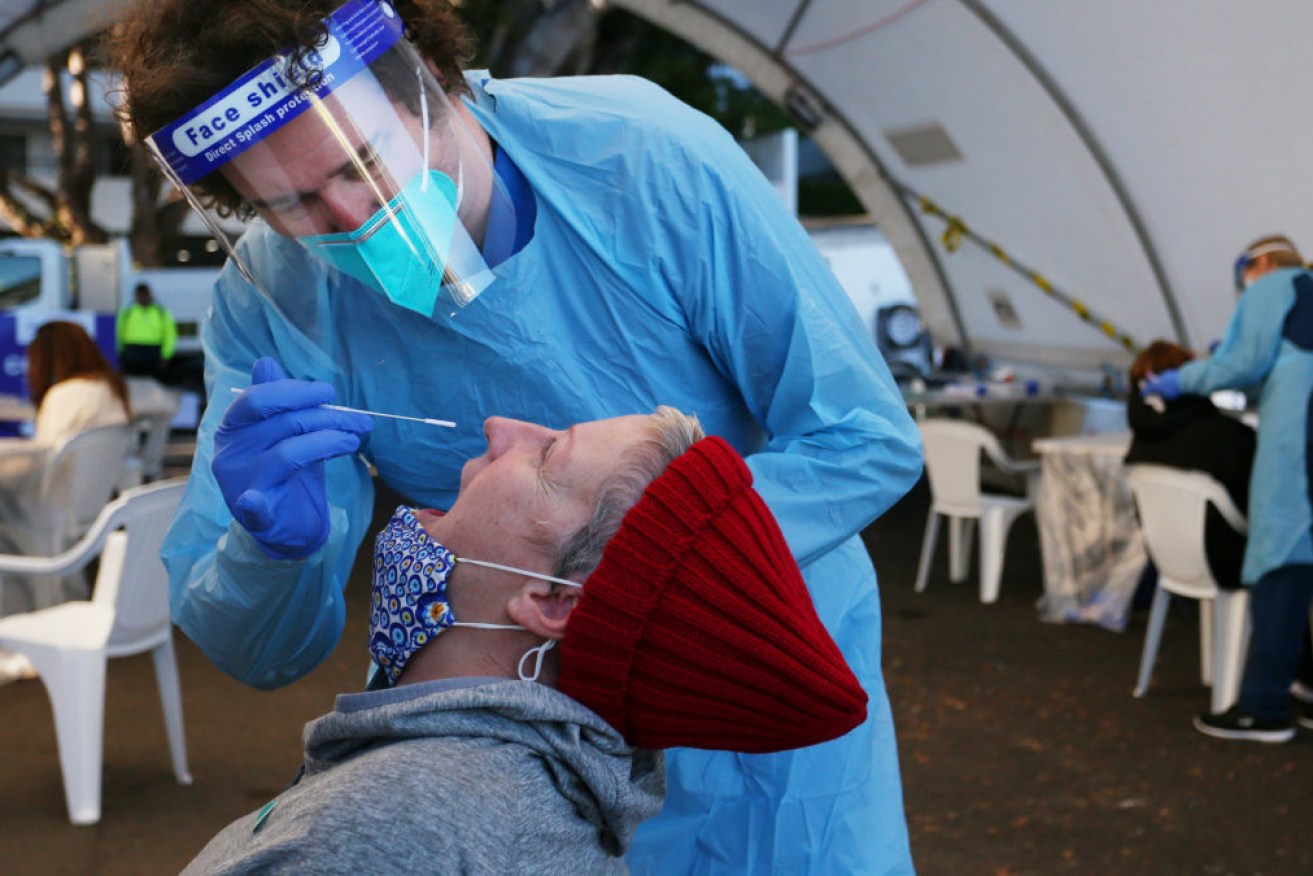
COVID testing, tracing and isolation will likely change as Australia's vaccination rates go up. Photo: Getty
Basic building blocks of Australia’s world-class contact tracing system could soon be radically altered, with quarantine times slashed, lists of exposure sites abandoned, and even COVID-positive people allowed to remain in the community under only basic rules.
Those are the predictions from some of Australia’s leading epidemiologists, who predict governments could make drastic changes to contact tracing, testing and quarantine once adult vaccination rates go beyond 80 per cent.
On the chopping block could be pleas to get a test at the slightest sniffle, and strict orders to isolate after a potential COVID exposure. In their place could be rapid test kits at work, highly-targeted screening at hot zones, and looser rules about isolating – even for those infected with COVID.
“The virus is entering a new era,” Mary-Louise McLaws, University of NSW epidemiologist and World Health Organisation advisor, told The New Daily.

Epidemiologists expect large scale COVID testing won’t be used in future. Photo: AAP
“Eventually, when we get greater vaccination rates and mRNA vaccines able to tweak more rapidly, we’ll settle into the idea that COVID is an immunisable and vaccinatable disease like whooping cough or tuberculosis.”
Catherine Bennett, Deakin University’s chair in epidemiology, agreed.
“The contact tracing has to change if you’re not trying to find every case,” Professor Bennett said.
“You don’t need to go upstream to find where they got it from. You’re not trying to link every case anymore.”
A change in mindset
To be clear, don’t delete the QR check-in app off your phone just yet. Contact tracing, check-ins and isolation are likely to remain a feature of Australian life for some time to come; especially in states with low or no COVID.
The Doherty Institute modelling, which underpins the national reopening plan, also stresses contact tracing is a key factor as Australia begins to slowly reopen.
But epidemiologists believe that, once the country hits vaccination rates above 80 per cent and the national strategy shifts from total ‘elimination’ of the virus into a looser mindset of ‘suppression’, the more stringent tendrils of the contact tracing system could be slightly relaxed.
Phase D of the national reopening plan, at vaccine threshold above 80 per cent, sets out a goal to “manage COVID-19 consistent with public health management of other infectious diseases” – which is when more easing of contact tracing and isolation may come into force, pending decisions of each state government.
The epidemiologists, leaning on scholarly work and experiences from other nations further along the COVID reopening path than Australia, made some predictions about where things would go.

Contact tracing will change, epidemiologist Catherine Bennett says. Photo: AAP
No longer aiming to track down every single contact of a COVID case means some of the basic contact tracing measures may no longer be needed, said Professor Bennett.
“What we expect to change is the circle of close contacts you bother to follow up,” she told TND.
“If it’s someone in a risky workplace, with people who don’t have a good immune response or in a non-vaccinated workplace, we should test those people to make sure they’re OK. But in other cases, they might say ‘you’re a contact, you don’t need to do anything now, but get tested tomorrow to assess the situation’.”
Isolation and exposure sites
Professor McLaws has already suggested hotel quarantine for returning travellers be replaced by home quarantine, for as little as five days instead of the current 14.
Professor Bennett believes changes could possibly extend to not even requiring COVID-infected people to isolate, or perhaps for only a week rather than the current fortnight.
The focus once vaccination levels are very high, she expected, would shift from trying to quarantine every case, to “finding where you need to intervene”.
“If you’re positive, it might not have any implications for you, besides having to monitor your health,” Professor Bennett said.
“If your risk of being infected is two-thirds less [from vaccination], it allows us to be less worried about missing the odd case, because the infection will likely die out.”

Things will change once vaccination rates go beyond 80 per cent. Photo: AAP
She believed lists of exposure sites would be vastly scaled back, with “tier two” sites likely to be discarded and fewer requirements on people at “tier one” sites.
“If you’re at an exposure site, maybe there’s still testing but you may not need to isolate until the result, or maybe it’s a rapid antigen test,” Professor Bennett theorised.
“For tier one sites now, the list could be thousands of people and you find 100 cases. In future, it’ll be trying to make that a bit more precise. There’s a risk you miss people if the net is smaller, but it’s important to find the balance between disruption and managing and outbreak.”
Testing changes
Rapid antigen tests at public sites or workplaces are likely to greatly expand. There’s also the potential for at-home tests for people with mild or no symptoms, with COVID-positive people recommended to avoid work or public areas for a few days – similar to current cold or flu recommendations.
The United States is already massively investing in at-home testing, with President Joe Biden outlining this measure among his latest vaccine plans.
Professor Bennett expected current testing to switch into ‘screening’ or ‘surveillance’ mode, with more targeted tests in problem or vulnerable areas. That could include swabbing international arrivals at airports to monitor if a new COVID variant was making its way in from overseas, or workplace testing at aged care homes or schools.
Areas with lower vaccination rates, or more vulnerable populations, may have more targeted ongoing testing.
Woolworths has begun introducing rapid antigen testing – less invasive than current PCR nose swabs, and with results in minutes not hours – into its distribution centres. Such tests could be rolled out, as seen overseas, at concerts, sporting matches or restaurants, with a negative result required for entry.
Tweet from @MarylouiseMcla1
Alexandra Martiniuk, epidemiologist at the University of Sydney, believed contact tracing would remain for some time. She noted contact tracing was still used to respond to diseases like measles, but said it would be tricky to keep using it for COVID.
“Contact tracing can reduce burden of infection in a population and likely still has merits even with high vaccination rates,” Professor Martiniuk told TND.
“We know that vaccinated people can still become infected and spread COVID and can have mild disease – sometimes even unaware they are infected. This certainly causes us different challenges.”
Scaling back contact tracing
Professor McLaws hoped to see vaccination rates above 80 per cent before significantly easing any COVID rules, especially for the under-40 age group which she said was “acquiring and driving” recent outbreaks in Sydney and Melbourne.
She also expected contact tracing would scale back on a general level, with less likelihood of – or need for – government or health officials to ask citizens to “get tested at the mildest of symptoms”. But she said contact tracing and testing would still play a key role going forward, albeit in a more targeted manner in specific settings.
“Testing may not go into hyperdrive like they have been in the past. They may target testing for areas of vulnerability and remove the person who’s the source, to stem further spread into vulnerable areas,” Professor McLaws predicted.
“In future, I can’t see how they will be able to do big callouts for testing, but they will be able to do callouts for people to get vaccinated if you’re in a hotspot.”
NSW Chief Health Officer Kerry Chant alluded to this on Thursday, saying the health department was “looking at what contact tracing looks like” once the state starts exiting lockdown. She mentioned possible changes to treatment of close and casual contacts, and how long people are required to isolate.
“If we have a positive case there, our response may be different if we know that people are fully vaccinated,” Dr Chant said.
“We are going to have to work on a number of those things and redesign what our test, trace and isolate policies are.”
Premier Gladys Berejiklian hinted at how NSW would respond to future concerning outbreaks, like regional towns with less health infrastructure, saying there could be rules barring entry or exit from the area. The more localised rules wouldn’t be a lockdown, with people in that town able to go about their lives, but essentially a quarantining of the area from the rest of the state.
Surveillance, not elimination
Professor Bennett compared the future of COVID treatment to how flu or even food-borne diseases like salmonella are managed. This could include ‘sentinel surveillance’, or random testing of otherwise healthy people who present to doctors.
“Like influenza, if people have symptoms then we test then, but we also try to have a finger on the pulse to see if ‘flu season’ has started and what variants are in the community,” she said.
Professor McLaws said she disliked the term “living with COVID”, instead preferring the idea of “working with” the virus. This, she said, would include updating standard protocols around isolation, quarantine and testing.
She warned it was likely that, once most people are fully vaccinated and many begin to ease off their alarm over the virus, compliance with testing callouts or willingness to isolate after a fleeting exposure may dwindle.

Mandatory quarantine could also come to an end. Photo: AAP
“It has the potential for breaking down otherwise. I can understand why the NSW Premier wants to open up … if I were leading this, I’d want to give people some reprieve,” Professor McLaws said.
She said there may come a time when more stringent measures are needed again – like in the event of a new variant emerging, or a particularly troubling outbreak at a vulnerable location – so she said it was important to foster goodwill in the community again.
“You want long-term cooperation if things turn nasty. You need to validate people’s experince and give them time to relax, so their cooperation will come back if there’s a new variant,” Professor McLaws said.
‘More about balance’
Professor Bennett echoed similar thoughts.
“I do think we learn a more sustainable approach to things. You risk people not complying, by asking too much and overplaying the risk card,” she said.
“We need to understand more about balance, minimal disruption versus control. I think it will be more about monitoring, less about worrying about every case, but closing down outbreaks by finding places where people are vulnerable.”
Professor Bennett said she expected low-level measures that had become “habitual”, like social distancing and mask-wearing and greater focus on staying home when sick, would remain well into the future.
Dr Chant said it would not “be a set-and-forget”, alluding to possible constant change on how those systems work. Professor McLaws said she believed that, even post-reopening, there will likely be constant shifts in rules, as new variants develop or new infection trends emerge.
“We’ll all need to live with uncertainty,” she said.
“I think it’s important to stress we need to start accepting uncertainty. The pre-COVID life won’t come back immediately, although it will come back. But for the next few years, we’ll have to deal with uncertainty like we never have before.”
Want to see more stories from The New Daily in your Google search results?
- Click here to set The New Daily as a preferred source.
- Tick the box next to "The New Daily". That's it.








