Australia now has fewer staffed ICU beds than at the beginning of the pandemic

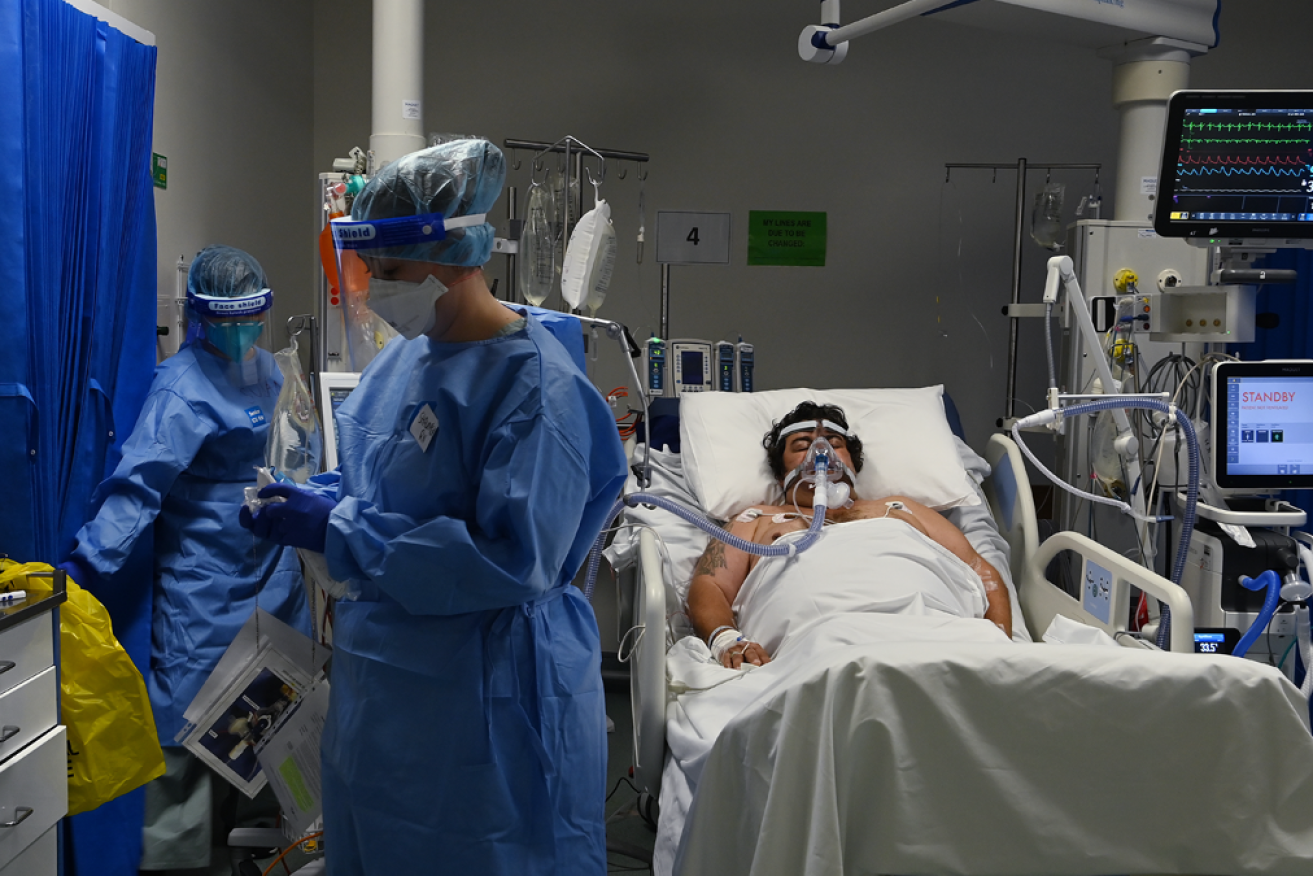
Hospitalisations are down across Australia, except in hard-hit Western Australia.Photo: AAP
A survey of every intensive care unit across Australia has found that there are now fewer staffed beds than there were at the start of the pandemic.
A team of researchers counted 2183 staffed ICU beds, down 195 from 12 months ago, and it’s a number that could constrain surge capacity during serious COVID outbreaks.
“Last year, we were worried about beds and equipment, but actually the equipment’s definitely been sorted. We have enough ventilators now,” lead researcher Dr Ed Litton told The New Daily.
“The very limiting step to our ability to increase our capacity to respond is staff – critically trained nurses.”
Dr Litton, a clinical associate professor at the University of Western Australia, was one of the team of 13 researchers from around Australia.
Although various state governments have touted their surge capacity in recent outbreaks, the researchers found there are only enough qualified staff to operate roughly half of the extra physical capacity of ICUs nationwide.
There aren’t enough staff to cover the 2627 additional surge beds outside of intensive care units.
“All else being equal, starting from a lower baseline of ICU beds is going to make responding more challenging, and potentially put more strain on the system,” Dr Litton said.
The biggest decrease in ICU capacity was seen in regional areas and in private hospitals.
Part of this has to do with the general upheaval of the pandemic.
Regional hospitals in particular have smaller pools of staff to draw upon, so when nurses are dispatched to vaccine clinics or other staff contract COVID-19 and have to take time off, they are difficult to replace.
Juggling beds
Despite the smaller number of staffed ICU beds compared to last year, Australian hospitals have adapted in other ways to the demands of the pandemic.
States have routinely cancelled elective surgery during major outbreaks, and this has freed up beds and staff who overlap with ICU wards.
“A really substantial proportion of the workload of intensive care is looking after patients after major elective surgery,” Dr Litton said.
However, COVID patients in intensive care may continue to take up beds that would otherwise be needed by other patients, such as car crash survivors.
“They are younger, they are staying in intensive care for longer, and they are needing care that can’t be provided anywhere else in the ward,” Dr Nhi Nguyen, an intensive care specialist from Sydney’s Nepean Hospital, told reporters in August.
Dr Nguyen also contributed to the research on ICU capacity.

Inside the intensive care unit of St Vincent’s Hospital in Sydney. Photo: AAP
The way forward
Throughout the pandemic, intensive care units have depended on nurses, doctors and other critical care staff working in unprecedented conditions.
“I’m confident that they’ll continue to rise to the challenge,” Dr Litton said.
“So one of the things that concerns me is the sustainability – that people rise to the challenge because they’re not going to step away in a crisis.
“But this is a disease that has become endemic and requires really a whole change in the approach to the critical care workforce.”
Many ICU staff are now experiencing burnout, anxiety or even traumatic stress.
Dr Litton said that health authorities need to make sure that this line of work remains an attractive career prospect, as well as to support ICU staff with the various stresses of the pandemic.
“How do we ensure it’s resourced appropriately to ensure that we’re ready for future surges?” he asked.
“Other places around the world are on their fourth or fifth wave, and there’ll be more pandemics in future.”








