Coronavirus panic-buying may force GPs, dentists to shut their doors

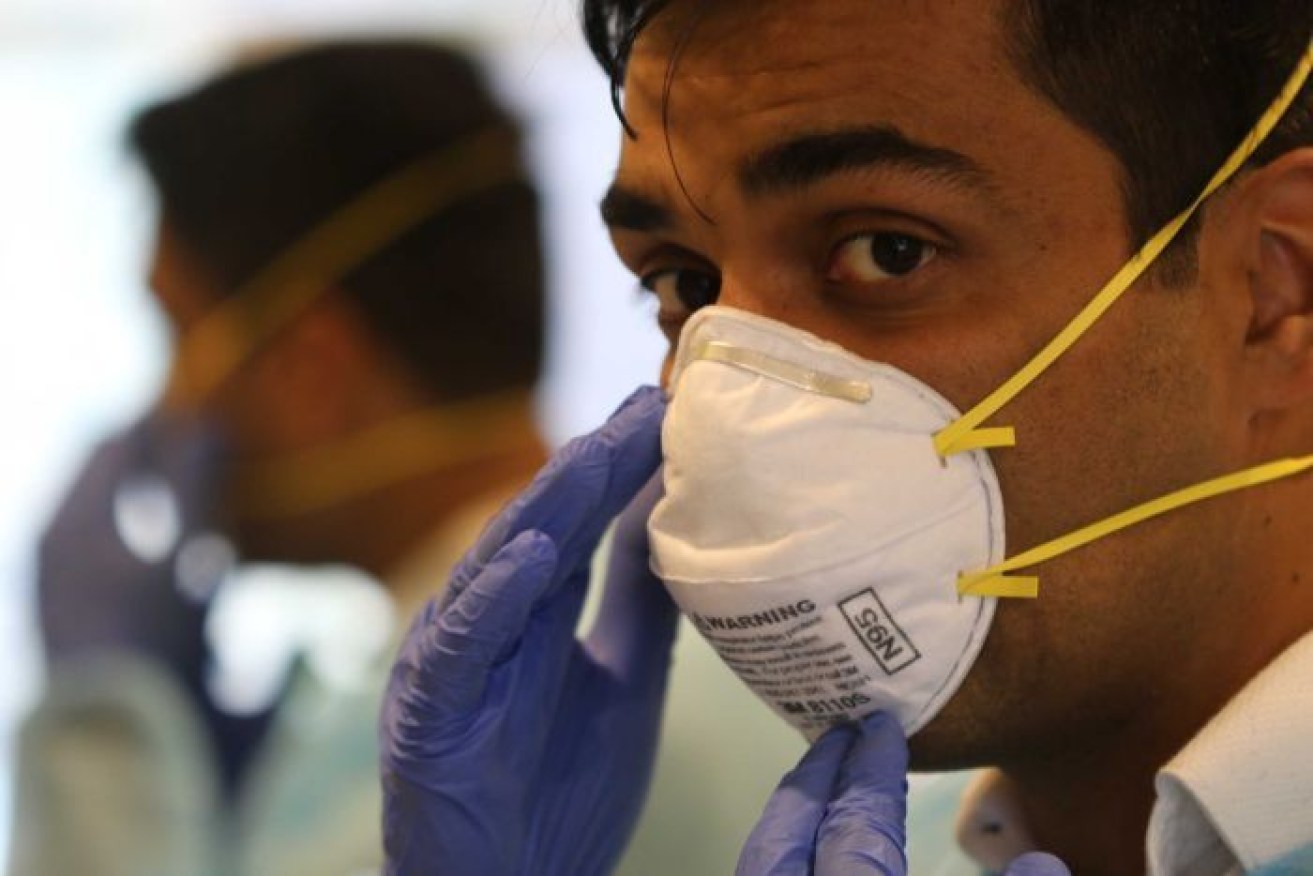
GP Vyom Sharma says masks are being rationed in some practices. Photo: ABC
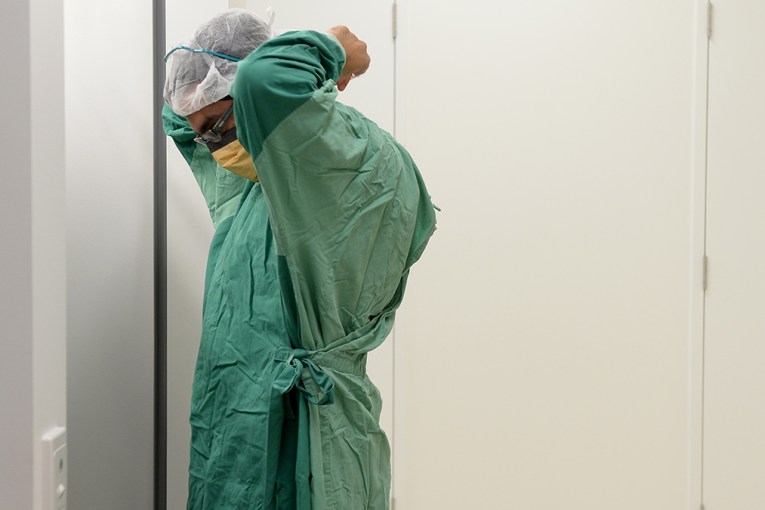
Dentists and GPs say “critically low levels” of vital surgical supplies such as face masks – brought on by frenzied buying amid the coronavirus outbreak – might force them to shut practices.
The Australian Dental Association said practices across the nation were expected to run out of masks within four weeks, because of the extraordinary demand brought on by COVID-19.
“Without surgical masks, dentists cannot treat patients safely and we run the risk of people going without treatment,” ADA deputy chief Eithne Irving told the ABC.
The association said Australia’s dental practices used millions of masks a month. New masks are used for each patient.
Meanwhile, desperate GPs say they are resorting to shopping at Bunnings to buy face masks to guard against the virus because too few government supplies are getting to clinics and traditional stockists have sold out.
Doctors are also relying on Twitter and Facebook to stay informed about the outbreak because, they say, official government communication is inconsistent and unclear.

Dentists are thought to have only four weeks of masks left. Photo: ABC
The risks to health workers have been highlighted after 40 staff from Sydney’s Ryde Hospital were ordered into home quarantine because of their interaction with a doctor later diagnosed with the virus.
NSW Health is also tracing 30 doctors who have had contact with the 53-year-old, including 12 who had close contact.
Some 24 nurses had contact with the doctor and of them 21 who had close contact. Authorities have contacted 21 of 37 patients.
In addition, staff at a Sydney aged-care home have called in sick en masse. A 95-year-old woman at Dorothy Henderson Lodge died on Monday, becoming Australia’s second confirmed COVID-19 death.
NSW Health Minister Brad Hazzard said his department had to cobble together staff for the lodge, once it became clear existing workers wouldn’t be turning up, fearful of becoming infected themselves.
Almost 50 people have tested positive for coronavirus across Australia, and the government has stepped up efforts to avoid outbreaks in aged-care facilities.
Royal Australian College of GPs president Harry Nespolon said the incident with the infected doctor underlined the “fragility of the healthcare system”.
“If we were to take 40 people out of every hospital, that’s a large amount of healthcare workers that won’t be available to take care of patients,” he told the ABC.
“There just isn’t another 40 people just sitting around there waiting to take their place.”
Tweet from @PrepWestBurbs
Dr Nespolon said GPs were not getting enough support, including equipment such as masks and gowns, to deal with an expected rush of patients and help under-pressure hospitals.
“I’ve certainly heard of GPs going to Bunnings to try and buy masks,” he said.
“We would rather that healthcare facilities had healthcare-standard masks and that we don’t have to resort to workarounds.
“It just underlines the importance of the Government supplying the masks and other personal protection equipment, not only to general practitioners but also, for example, aged care facilities.”
In late January, the government authorised the release of a million masks from the national medical stockpile, to be distributed to doctors and health workers via local primary health networks.
But several GPs have told the ABC it has still been very difficult to get the masks. Suppliers are sold out, and masks from the national stockpile
Melbourne GP Vyom Sharma told the ABC some GPs were essentially “rationing” masks to avoid running out before an influx of coronavirus cases.
“Getting our hands on masks has been tricky, to say the least,” Dr Sharma said.
“Just for one patient, we might have to go through four masks, and we’ve only got about 50 in our reserve.
“We realised very early on that we’d have to source our own masks.”