Restricting access to opioids could drive pain sufferers to buy harder drugs, experts warn
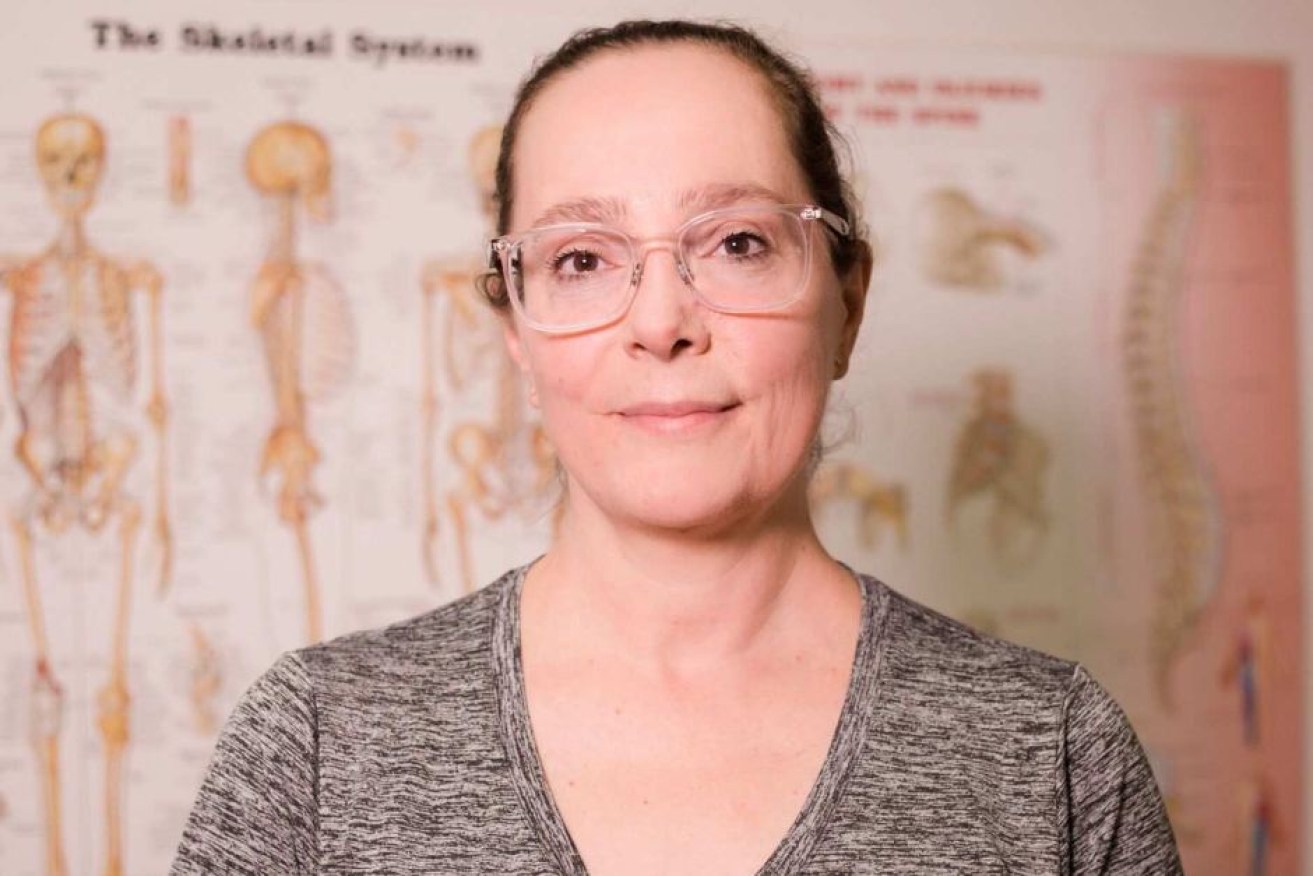
Leah Dwyer has suffered chronic pain for a decade, but says kicking codeine was the hardest thing she's ever done. Photo: ABC News
Australia has been warned that moves to restrict access to addictive opioid painkillers could drive pain sufferers to illegal markets or even stronger substances, if people are not able to access affordable, effective options to manage their pain.
The federal government says it has written to 4800 doctors to let them know they could be prescribing too many doses of addictive painkillers, as it seeks to avoid an opioid crisis like that seen currently in the United States.
Health Minister Greg Hunt said the letter was intended to let the top 20 per cent of prescribers know where they sit, in the hope they will moderate or regulate their actions.
The move follows on from changes the government made to regulations in February that tightened access to the painkillers by making all codeine products available only with a doctor’s prescription.
Low-dose codeine was previously available over the counter in pharmacies.
“We don’t want to end up in the place that the United States is in where opioids are a national crisis,” Mr Hunt said.

Health Minister Greg Hunt said Australia did not want to end up in a situation where opioids are a national crisis. Photo: ABC News
Chronic pain sufferer Leah Dwyer recently managed to break her addiction to codeine, but she reckoned she could have found a doctor to prescribe the drug.
“Any doctor probably would have said, “With your condition, yes, it’s very painful, there aren’t many treatments, you’ve tried all the treatments. Here’s some codeine,” she said.
For every day of the past 10 years, Ms Dwyer has experienced a level of pain in her neck that she describes as 12 to 15 out of 10.
Her neck muscles constantly spasm, leading to a slight tremor, and the pain has often been so bad she would sit in her car crying for 15 minutes after work before she could drive home.
She describes kicking her codeine habit as the hardest thing she has ever been through.
“Shaking, even more than I’m shaking now. A massive escalation of pain, sweating, sleeplessness,” she said.
She was lucky to have a friendly pharmacist just a few doors down from where she worked, and together they worked out a plan for her to taper off the opiate. But it was a long, difficult road, and she almost gave up several times.
“Many mornings I woke up and thought, ‘OK, you’ve got until February. It’s only September. I’ll do it again, just not right now’,” she said.
Her pharmacists helped her stay on track, but hers could have been a very different story.
A recent report in the British Medical Journal has shown that when the US Drug Enforcement Administration made it harder for people to get hold of hydrocodone, many people did not break their addictions. Instead, they turned to illegal suppliers.
Almost as soon as the tightened rules came into force, there was an approximate doubling of the prescription opioids being traded over the dark net in the US.
‘Cheap, very accessible and it worked’
But even more worrying is that many people opted for stronger options.
Criminologist Dr James Martin from Swinburne University said the data his team gathered from the dark web showed people did not simply switch from buying the drug legally to buying it on the black market.
“What we saw is people opting for more potent and more dangerous types of prescription opioid, so initially a rise in oxycodone, and more troublingly a very significant increase in the use of fentanyl, which is a very powerful synthetic opioid,” he said.
In criminology, this is known as ‘the iron law of prohibition’ which argues that if you ban or restrict access to a substance, people will seek it out on the black market, and when they do they will opt for harder tack.
Dr Martin pointed out that this was demonstrated in the US during prohibition, as people who would normally have drunk beer or wine switched instead to more potent substitutes, such as whiskey or gin.
He said a similar effect was being seen in the US with the opioid crisis.
“If you cut off people’s legal supply of prescription opioids then they are starting to shift towards more potent opioids, such as oxycodone and fentanyl, and increasing rather than decreasing the amount of harms associated with those drugs,” he said.
It is too early to tell whether people in Australia who have become dependent on codeine have begun seeking it out on the black market. But experts are warning that restricting the supply of these painkillers, without effectively addressing demand, might not work.
Painaustralia advocates on behalf of people living with pain, and wants to see that those people are able to get access to the best quality of care at an affordable price.
“If that doesn’t happen, we may see unintended consequences like people using higher-level opioids, or other medications, or trying to self-manage, but poorly,” Painaustralia’s CEO Carol Bennett said.
Many pain sufferers are just looking for a treatment that allows them to cope on a daily basis.
For Leah, she thought she had found that when she discovered codeine.
“For the first time in two years, I slept through the night and I thought, ‘Hallelujah, this is it!’,” she said.
“It just went from there. It was cheap. It was at every single pharmacy, and it was just very, very accessible. And it worked.”
Level of opioid use ‘higher than it should be’
Leah’s experience is not unique.
“The level of opioid use in Australia is much higher than it should be,” Ms Bennett said.
Although Mr Hunt insists that Australia has the best doctors in the world, it is clear the government now sees some doctors as contributing to the problem.
It has confirmed that one country doctor prescribed more than 68,000 doses of opioids in less than a year, and another doctor in a city wrote prescriptions for more than 56,000 doses over 12 months.
Given that until February low-dose codeine was available without a prescription, those doses are likely to have been for stronger opioids.
Ms Bennett said that to avoid unintended consequences from tightening the access to these painkillers, Australia needed to deal with the full complexity of treating pain.
“What this [is] about is better awareness of the options for managing chronic pain, both by consumers, but also by health professionals,” she said.
She said she wanted to see all Australians have better access to affordable options, such as physiotherapy, psychological support and massage.
While admitting that delivering these services in regional and rural areas was a challenge, she said there were models for delivering specialist pain treatments that had been shown to work.
“We just need to prioritise those models and invest in them,” she said.
Dr Martin said his research showed that if governments used supply-side restrictions such as tightening regulations, but did not put in place other measures to reduce either the demand for the drugs, or the harm they cause, then their policies were at risk of not achieving their goals.
“There is a whole cohort of patients out there who have developed habitual or addictive relationships with these drugs,” he said.
“Simply changing their supply doesn’t actually address those demand and addiction problems.”