One chance in 12 any hospital bed holds a COVID patient
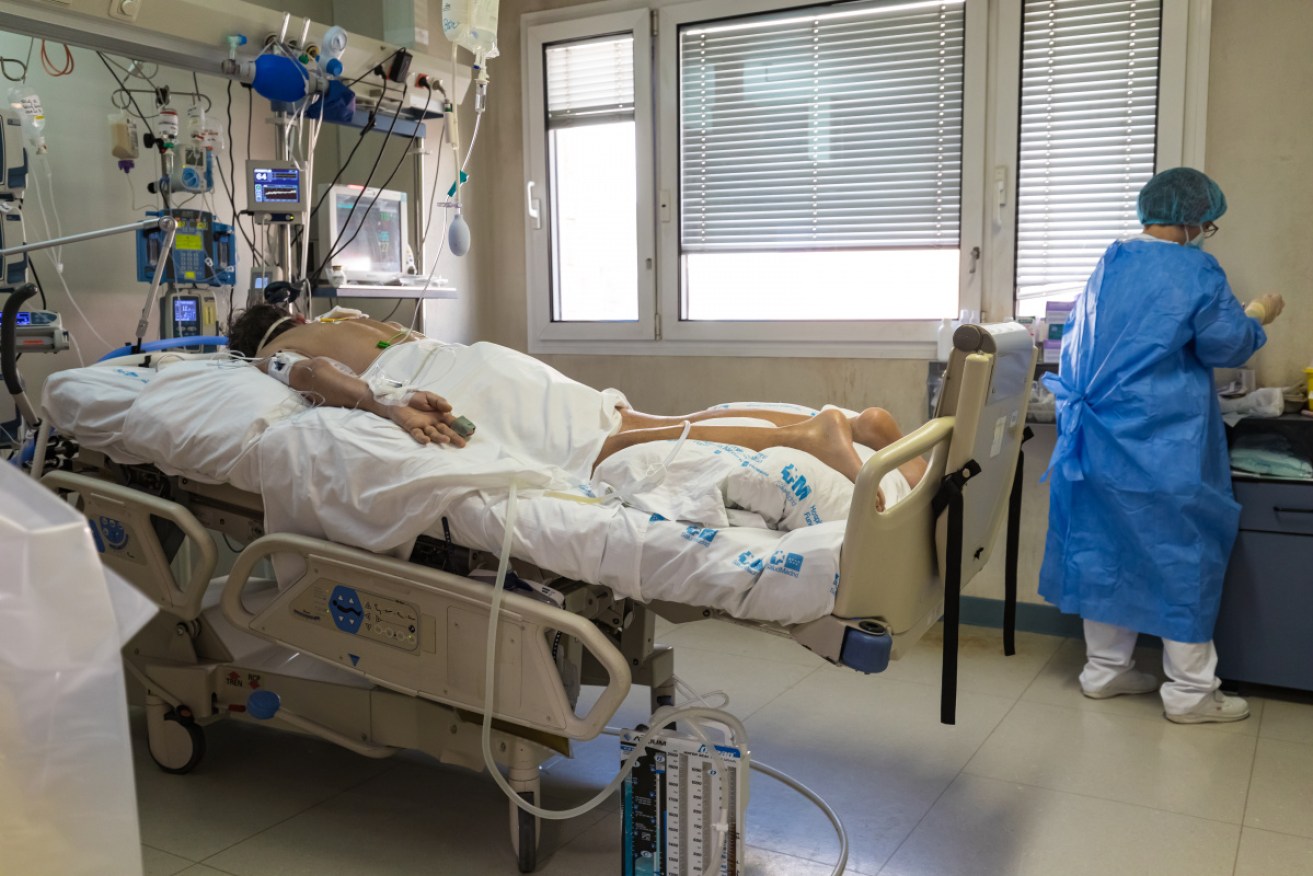
The number of patients in intensive care has seen a welcome drop, but hospitals are still trying to cope. Photo: AAP Photo: Getty
One in 12 public hospital beds across Australia is occupied by a COVID-19 patient despite fewer people ending up in intensive care than during previous waves of the virus.
Hospitals nationwide are “heaving” under the coronavirus caseload, with more than 5000 beds occupied by positive patients, Health Minister Mark Butler says.
“We’re numbering about 330,000 cases on a seven-day average per week at the moment, but we know from sampling from the positivity rates that we’re getting for PCR tests, that the real number is probably at least twice that,” he told the Australian Medical Association national conference on Saturday.
‘Extraordinary numbers’
“It is an extraordinary numbers of infections with this highly infectious new (Omicron) subvariant.”
Mr Butler said the one upside of the current Omicron wave was that ICU rates were well below where they were in January, while the number of flu cases was also declining sharply.
But he added that the take up of third vaccine doses had “stalled to quite an alarming extent”, with around five million people yet to receive a booster after their two initial shots.
Mr Butler’s comments came as a leading epidemiologist warned that authorities should take as much care with the air as they did with water in order to combat the latest COVID-19 surge.
Call for ventilation audits
Authorities should take as much care with the air as they do with their water to help combat the latest surge in COVID-19 cases and future waves, a leading epidemiologist says.
Adrian Esterman from the University of South Australia says better ventilation and better vaccines will be vital to fighting the virus over the long term.
Despite high numbers of active cases across the country, he questioned how many public buildings, offices, factories and retail settings had conducted ventilation audits and taken steps to improve their air conditioning.
“It’s the key. We wouldn’t start drinking contaminated water, yet we seem quite happy to breathe contaminated air,” Professor Esterman said.
“This is an airborne disease. Over 98 per cent of infections are airborne, probably even more than that.
“If it’s an airborne disease, why aren’t we looking after our air?”
While giving evidence to a South Australian parliamentary committee, Prof Esterman also urged the development of a US-style Centre for Disease Control to better coordinate pandemic efforts.
“One of the big problems with our approach to COVID-19 is that every state and territory does a different thing,” he said.
No national definitions
“Even things like the definition of a case. There’s hardly any national definitions or national approaches.
A good example is contact tracing, Professor Esterman told the committee, with each state and territory having their own method.
“This is a crazy situation. We need a national approach. It would benefit the whole country,” he said.
Prof Esterman noted the new federal Labor government had taken to the election a policy to establish an Australian CDC.
In policy documents, Labor said a local CDC would ensure ongoing pandemic preparedness, lead the federal response to future infectious disease outbreaks and work to prevent non-communicable as well as communicable diseases.
“Hopefully that will happen,” he said.
LATEST 24-HOUR COVID-19 DATA:
- NSW: 13,425 cases, 46 deaths, 2210 in hospital with 68 in ICU
- Victoria: 8937 cases, 61 deaths, 837 in hospital with 38 in ICU
- Queensland: 18,678 cases, no deaths, 861 in hospital with 30 in ICU
- WA: 4034 cases, 13 deaths, 417 in hospital with 15 in ICU
- SA: 2767 cases, four deaths, 335 in hospital with 10 in ICU
- Tasmania: 923 cases, one death, 144 in hospital with four in ICU
- ACT: 719 cases, two deaths, 152 in hospital with one in ICU
- NT: 303 cases, no deaths, 56 in hospital with none in ICU








