The no-jab Australian vaccine patch that could save the world from COVID and other nasties

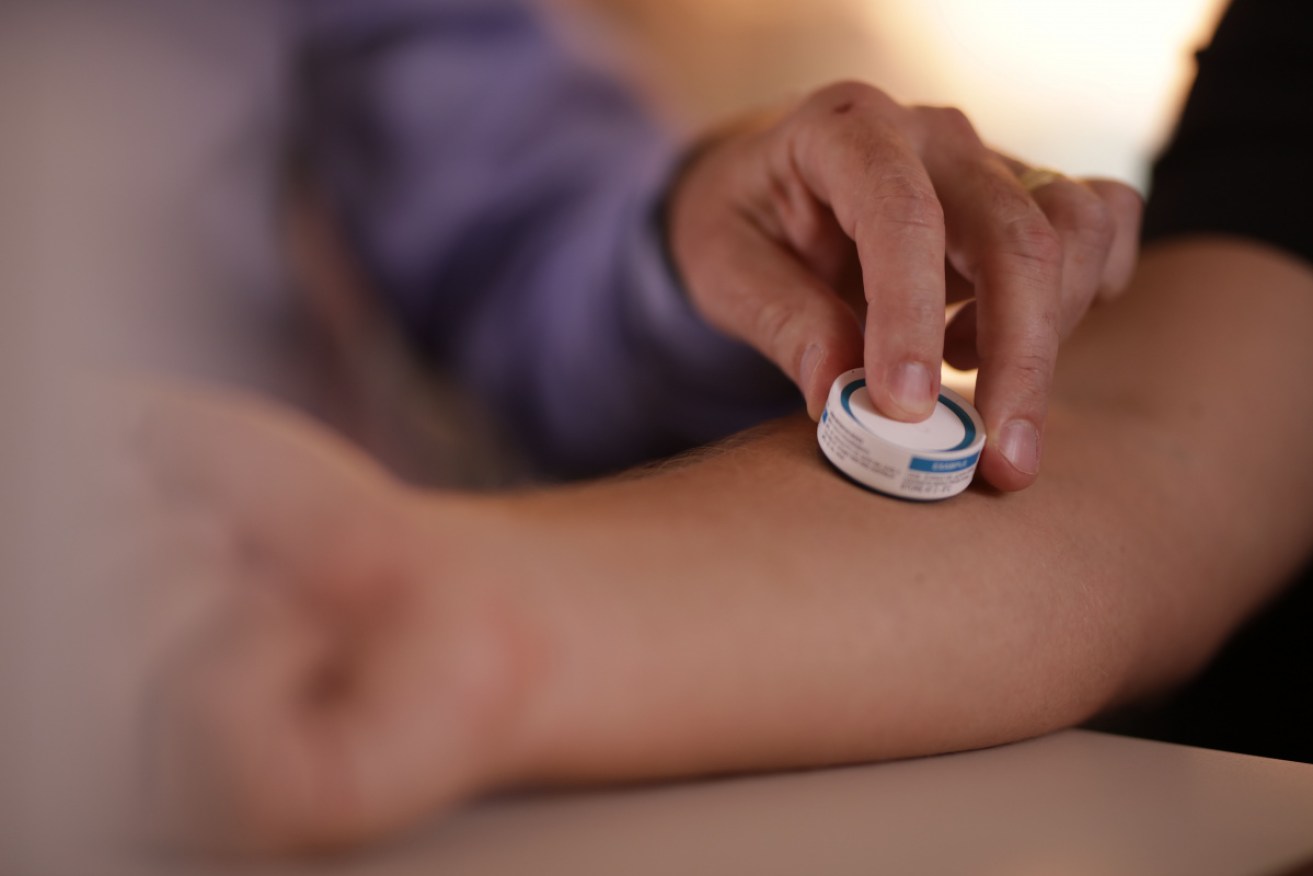
Researchers have developed patch that "almost imperceptibly" delivers vaccine into the skin. Photo: UQ
Australian researchers have developed a potential COVID-19 vaccine patch as an alternative to needles – an applicator containing 5000 microscopic projections that “almost imperceptibly” deliver vaccine into the skin.
This may sound like great news to people scared of injections, but the real value of the patch is in poorer countries – where vaccines are scarce, storage facilities are generally inadequate and variants are likely to multiply unchecked and spread around the world.
The plight of poorer countries is rarely top of mind in the West, but the pandemic is changing that. It’s clearly in everybody’s interest to get every human being vaccinated – if not COVID-19 will own our lives for decades.

A close-up of the patch. Photo: UQ
This week the World Health Organisation, World Trade Organisation and International Monetary Fund jointly called for a “stepped-up coordinated strategy, backed by new financing, to vaccinate the world”.
Money is one part of the solution. The other is technical innovation to solve the manufacturing and delivery challenges in places where health care is rudimentary – and where meeting cold-chain requirements can be highly problematic.
And this is where the vaccine patch, developed at the University of Queensland steps in. In tandem with a second generation COVID-19 vaccine from the University of Texas, the patch appears to solve these problems.
Promising partnership
First, some back story. There’s already considerable buzz about the new vaccine called NDV-HXP-S.
According to The New York Times, it’s the first COVID-19 vaccine to use “a new molecular design that is widely expected to create more potent antibodies than the current generation of vaccines”.
According to a statement from the University of Texas, the vaccine uses a highly stabilised spike protein from the surface of the coronavirus – dubbed HexaPro – in order to train the human immune system to recognise and fight infection.
The researchers say they designed HexaPro to be “a more stable antigen”.
In cell culture, this translated to a “more than tenfold increased yield relative to the first-generation spike constructs used in current vaccines”.
And where celebrated vaccines such as the Pfizer jab rely on expensive new-technology factories, NDV-HXP-S is made in chicken eggs, like the influenza vaccines produced in the billions every year.
In other words, it’s much easier and cheaper to make – which is great news for countries that can’t afford to build high-tech factories or meet the cold-chain requirements of leading-edge vaccines such as the Pfizer jab.
All of which led the Times to declare that the vaccine “could change how the world fights the pandemic”.
Tested in the real world yet?
NDV-HXP-S has started clinical trials in Mexico, Thailand and Vietnam, and is set to be trialled in Brazil.
If these run as quickly and positively as the trials that delivered the Pfizer, Moderna and AstraZeneca jabs, then NDV-HXP-S could be cleared for emergency use in a few months.
If it struggles like the promising but problematic Novovax vaccine to navigate successful trials, then … who knows?
And Africa will eventually be the big test. While influenza vaccines and antivirals are available there, population coverage is said to be very low – and many countries have political problems that could get in the way of a full rollout.
Still, this is more a very good news story than not.
What makes NDV-HXP-S a viable candidate in very poor countries is that it can be stored at 2-8 degrees Celsius – which means it could be transported in the kind of coolers you take to a picnic.
The patch amplifies the vaccine’s efficacy
In a new study, University of Queensland’s (UQ) high-density micro-array patch, known as HD-MAP, was used to vaccinate mice with NDV-HXP-S.
Dr David Muller, from UQ’s School of Chemistry and Molecular Biosciences, in a statement from the university said the vaccine patch produced strong immune responses that were shown to be effective when the mice were exposed to SARS-CoV-2.

Dr David Muller. Photo: UQ
“When the Hexapro vaccine is delivered via HD-MAP applicator – rather than a needle – it produces better and faster immune responses,” Dr Muller said.
“It also neutralises multiple variants, including the UK and South Africa variants.”
And of course “it’s much more user-friendly than a needle – you simply ‘click’ an applicator on the skin, and 5000 microscopic projections almost-imperceptibly deliver vaccine into the skin.”
But there was another impressive pay-off in the marriage between NDV-HXP-S and the HD-MAP applicator:
“We’ve shown this vaccine, when dry-coated on a patch, is stable for at least 30 days at 25 degrees Celsius and one week at 40 degrees, so it doesn’t have the cold chain requirements of some of the current options.”
So we’re ready rock, right?
The HD-MAP applicator is being commercialised by a company called Vaxxas, founded in 2011 by UQ’s commercialisation company, UniQuest.
The UQ team, together with Vaxxas, “hope to take the technology to the world and are looking for funding opportunities to accelerate to clinical trials as soon as possible”.
Fingers crossed.








