‘Forgotten and ignored’: Disability royal commission finds failure in pandemic response
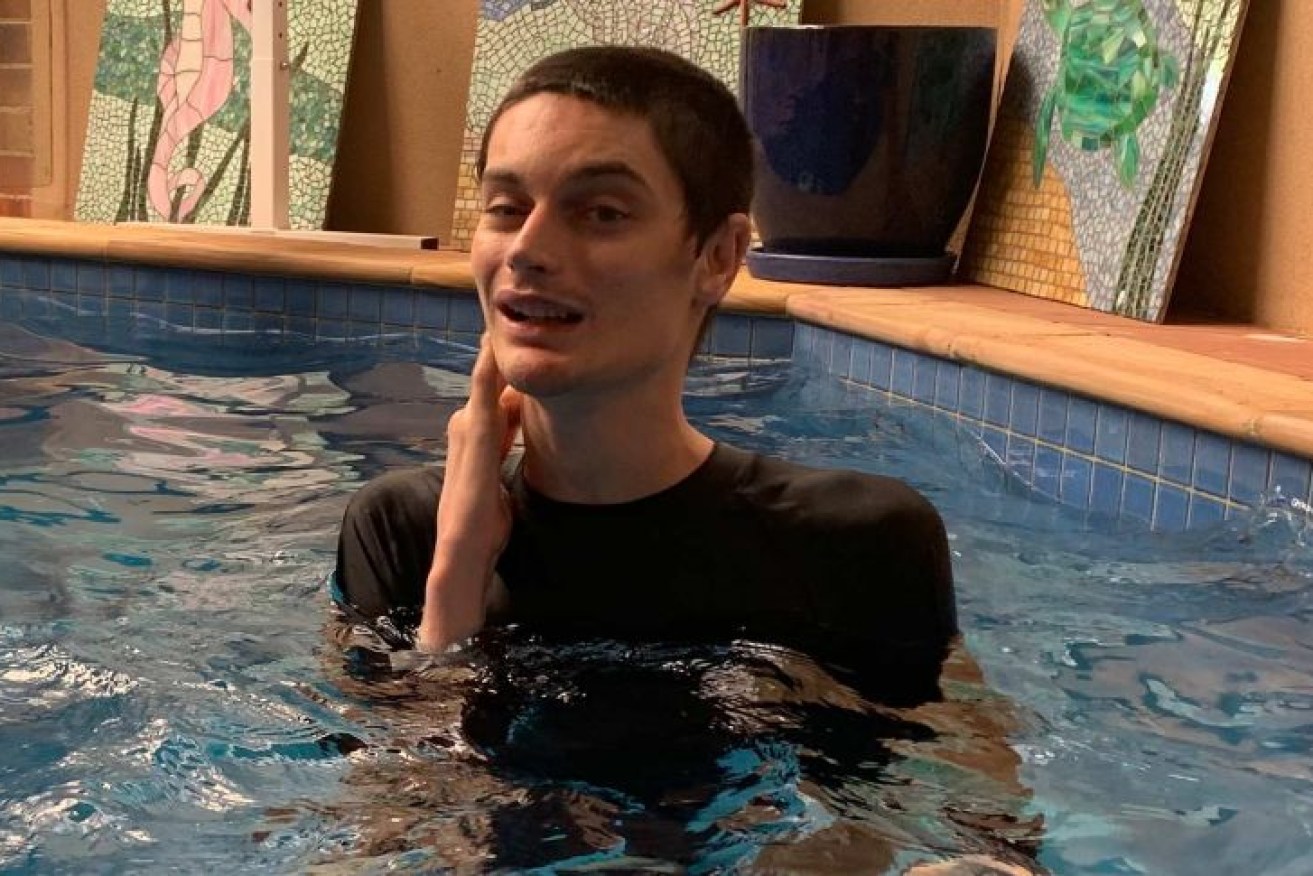
Jarrod McKenzie and his mother were left days without information or support when they were diagnosed with COVID-19. Photo: ABC News/Patrick Stone
People with disability have been “forgotten and ignored” during the pandemic, leaving them “stressed and frightened,” a Commonwealth report has found.
Disability royal commission Chair Ronald Sackville said the government was responsible for a “serious failure” in its communications with people living with disability.
The disability royal commission held a hearing with 36 witnesses in August into the impact of the pandemic on the disability community and on Monday its COVID-19 report was tabled in Parliament.
In it, the commission made 22 recommendations and Mr Sackville called on the federal government to consider them “very swiftly”.
“The recommendations are designed to ensure that for the future, people with disability are consulted from the very outset,” he said.
“It was the absence of that consultation that led to significant failures in the responses of the Australian government.”
Mr Sackville said there was no plan in place at the time the pandemic commenced that addressed the specific issues of people with disability.
“People were deprived of essential supports without warning and left without support and therefore bewildered, frightened and sometimes even without food or medication,” he said.
Mr Sackville said one of the “most disturbing” features of the commission’s inquiry was the lack of data on the number of people with disability who contracted COVID-19.
“Our recommendations include requiring the Commonwealth to make sure that data is collected and disseminated so that we know exactly what is happening within the disability community in this and any other emergency.”
The ABC has contacted the government for comment on the report.
‘Wild west’ NDIS providers chaotic
General manager of operations for ONCALL Group Australia Laura Green said a surge workforce of support workers had to meet “extraordinary requirements” during the pandemic, including: “Isolating between shifts and being able to isolate for the two weeks after they’d assisted someone with COVID-19.”
Workers also needed “qualifications and experience enough to be able to walk in to any new location and provide support to people that they had never met before”.

ONCALL’s Laura Green said a section of the NDIS operated like ‘the wild west’. Photo: ABC News/ Patrick Stone
Ms Green said the pandemic revealed a real divide in providers in the National Disability Insurance Scheme (NDIS).
“We had established providers who were working together,” she said.
“But there was a whole other section in the NDIS market, a little bit of the wild west … made up of small, new and unregistered providers, and that part of the market just went into chaos.”
We saw people failing to get their support needs met and we saw serious risk to people with disability and their families.”
She called on the federal government to create national minimum standards for support providers to follow.
Recommendations on PPE, standards
The disability royal commission’s report has recommended the NDIS Commission should review its practice standards.
It also recommended disability support workers receive priority access to personal protective equipment (PPE) and COVID-19 testing if there was a resurgence in the pandemic.
The first recommendation in the report has called on the Commonwealth to consider the findings and recommendations as a “matter of urgency.”
“This pandemic is not over… it may revive,” Mr Sackville said.
“We want the Government to respond very swiftly so that the pandemic is dealt with in a way that protects and safeguards the well-being, the safety, the health of people with disability, and we would expect a prompt response.”
The commission also found disability representative organisations (DROs) did not have enough funding during the pandemic to cope with increased demand for their services.
It recommended supplementary funding be immediately committed if there was a resurgence in infections.
Other recommendations from the report include that the Commonwealth Department of Health should establish a unit for developing plans to protect the health and well-being of people with disability during emergencies like the pandemic.
‘Who is going to look after him?’

When Karen McKenzie was diagnosed with COVID-19, she feared there would be no-one to look after her son. Photo: ABC News/Patrick Stone
Victorian mother Karen McKenzie and her severely autistic son Jarrod contracted COVID-19 in September from a support worker.
He initially contacted her to say he could not come to work as he had a sinus infection, but later sent a text message to confirm he had tested positive.
Ms McKenzie had already begun to feel unwell and testing confirmed she and Jarrod had also contracted COVID-19.
“It was a bit scary,” she said.
“My initial thought was well how sick are we going to get and am I going to be hospitalised and if I am, what’s going to happen to Jarrod? Who is going to look after him?”
Ms McKenzie and her 21-year-old son were left days without support and information.
They finally received help from ONCALL Group Australia, which provided three support workers over three weeks.
The disability royal commission is continuing its public hearings and is currently looking at the experience of First Nations people in the child protection system.








