‘Broken’ aged care system needs urgent reforms, unions demand

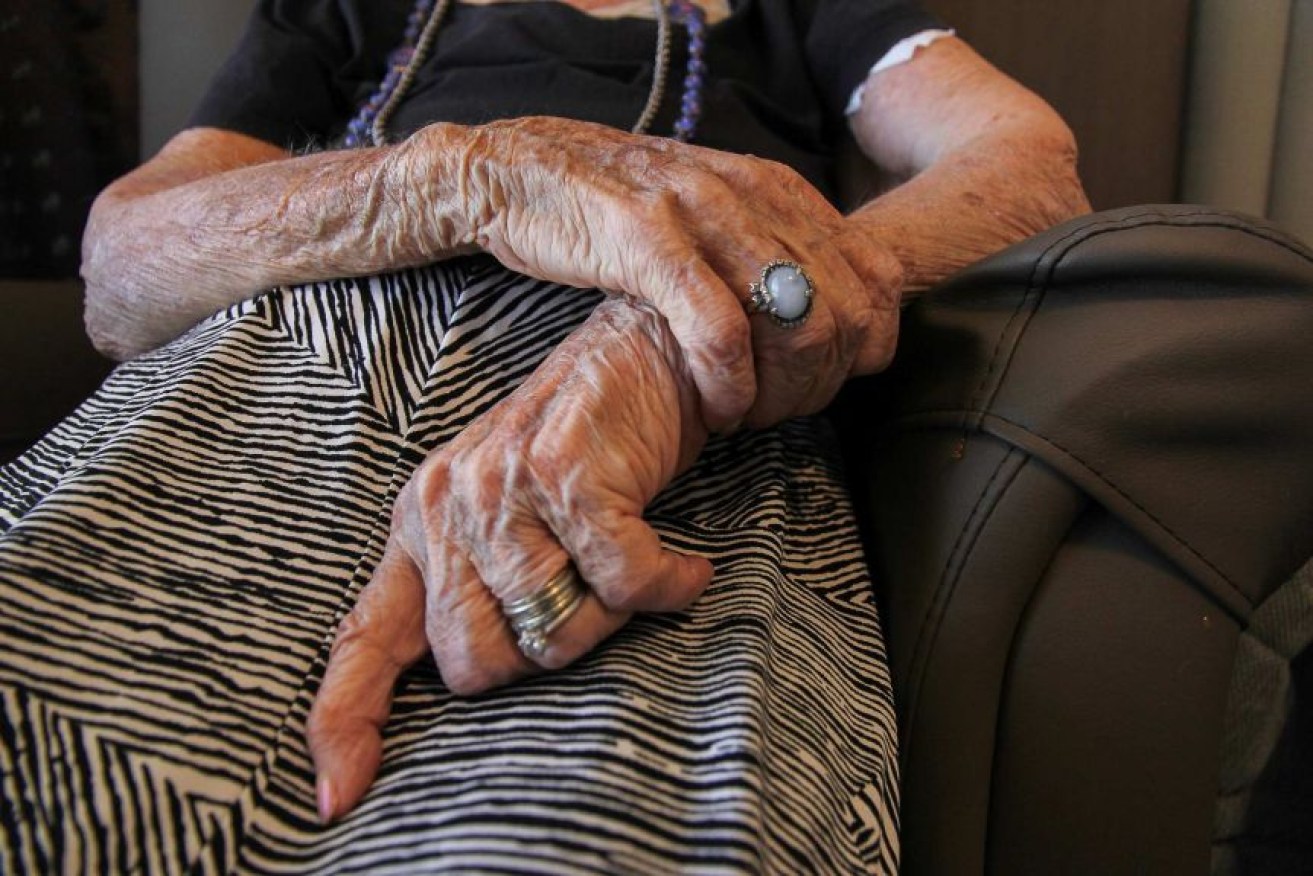
Unions have released a plan to "fix" aged care. Photo: ABC Central West
Aged care workers are so overworked they often don’t have time to talk to residents they are bathing, unions have claimed, in launching a comprehensive plan to fix the “broken” sector.
Workers in aged care would be forced to meet higher mandatory qualifications around infection control, under the ambitious trade union demands.
At least 633 COVID deaths have been linked to aged care homes in Australia, about three-quarters of the nation’s total virus toll. At least 4200 more residents and staff have been infected.
Countless horror stories from the sector have emerged in recent months; of poor or non-existent personal protective equipment usage, lapses in infection control and quarantine, failures in providing adequate healthcare, lack of inspections from regulators, and damning reports of elderly residents left without food, dressing or bathing.

Aged care has been hard hit by the coronavirus pandemic. Photo: AAP
On Monday, three trade unions representing aged care workers – the Health Services Union, the Australian Nursing and Midwifery Federation and the United Workers Union – and the Australian Council of Trade Unions released a suite of ideas they say are essential to protect residents and workers.
ACTU president Michele O’Neil called privatisation of aged care “a failed experiment” that had “failed working people and the people they care for”.
The unions want mandated minimum staffing levels to ensure residents are properly cared for, more transparency in government funding of homes, boosted mandatory training, including strengthened focus on infection control, and increased pay to retain skilled workers.
“Long before the COVID-19 pandemic began, and as exposed by the Aged Care Royal Commission, chronic and widespread understaffing across the aged care system had created unsafe environments for both workers and those they cared for,” ANMF federal secretary Annie Butler said.
“The pandemic has now revealed just how dangerous understaffing is, with tragic consequences for far too many older Australians and their families.”
Carolyn Smith, the UWU’s aged care director, said her members reported that understaffing and time pressures meant “timetables don’t allow them the simple humanity of pausing to have a chat with people as they prepare their shower”.

ACTU president Michele O’Neil. Photo: AAP
“Our members tell us every day they are forced to make the choice between completing their tasks or properly looking after those they care for,” she said, calling Australia’s aged care system broken.
“The pressures on aged care staff leaves our members demoralised and burnt out, and helps explain why Australia has one of the world’s worst staff retention rates in aged care.”
The unions’ Action for Aged Care policy calls for “a substantial increase in funding”, as well mandating a minimum amount of time each resident should receive in direct care from staff – requiring a boost to staff numbers.
“The amount of direct care time residents should receive, from a skills mix of staff, should be mandated under legislation,” the policy demands.
The unions also called on the federal parliament to institute laws to compel more transparency and provide records on how facilities use federal funding. This, they claim, would “ensure aged care providers are prevented from putting profit before people”.
The unions also criticised what they called an “absence of formalised minimum training and qualification standards” for workers in nursing homes, which they said “undermines the quality of care available”.
They are calling for a new training protocols and qualification standards in areas such as infection control, fall prevention, and caring for people with dementia.
The unions also demand “decent pay and enough hours to live on”, following reports that aged care workers who worked at multiple facilities may have unwittingly carried infection between their places of work.
“The pandemic has shown us that insecure and undervalued work leaves workers unable to provide the quality of care that older Australians should be able to expect,” Ms O’Neil said.

Unions want minimum staff levels in aged care. Photo: Getty
“We need to ensure that one job is enough for any worker in aged care. Aged care workers having to work between multiple facilities has been a huge problem during the pandemic and must end.”
Victorian Premier Daniel Andrews on Monday voiced support for the types of measures flagged in the campaign, saying increased staffing levels could assist.
“I think there are underlying risks in private aged care today and we are working very, very hard to make sure we have a system in place that keeps those settings as safe as possible until a vaccine comes,” he said, saying aged care homes would “remain very risky places.
However, Mr Andrews said his government did not have the power to mandate such measures, hinting the federal government might be lobbied instead.
“We do not run those places. I do not pay the staff, they are not accountable to me but we will be checking and monitoring and making sure every aged care facility is as safe as possible,” he said.
Federal Labor education spokeswoman Tanya Plibersek also backed some of the recommendations, calling on the government to take action.
“They need to restore the funding. They need to look at staffing levels, careers for people who work in aged care, making sure that there are the skilled, qualified staff available to properly look after every older person,” she said.