Is expensive robotic surgery for prostate cancer better?
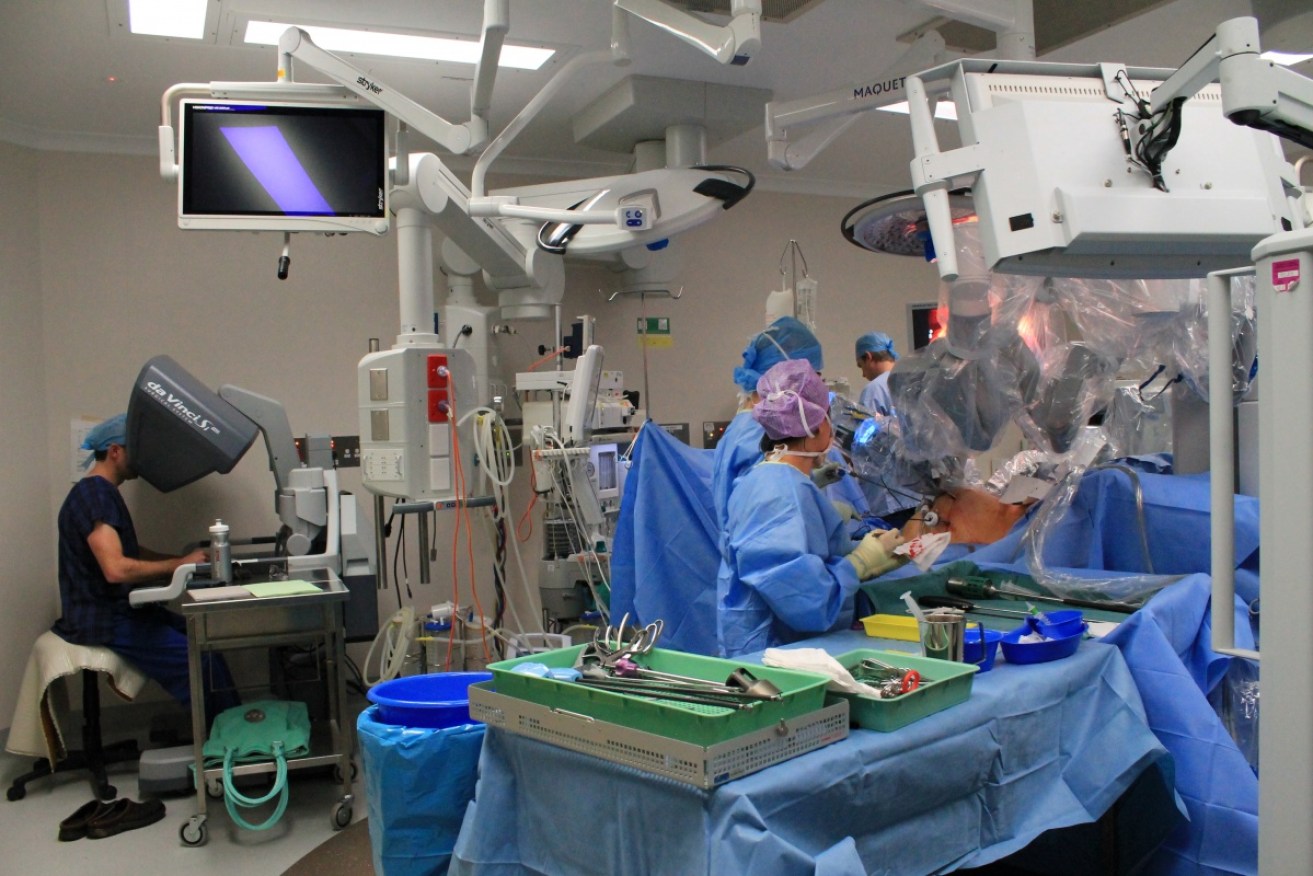
Robotic surgery is giving prostate cancer patients another option to traditional surgical procedures. Photo: Griffith University
As the popularity of robotic-assisted prostate surgery grows, experts are questioning its benefit to patients and how it compares to traditional open surgery.
A recent study, led by Queensland researchers, compared the health outcomes of open prostate surgery with robot-assisted surgery in 296 men and followed their progress over a two-year period.
Publishing their results in The Lancet Oncology, the researchers found both techniques were equally successful at maintaining urinary and sexual function at six, 12 and 24 months following the procedures.
Robotic-assisted technology is less invasive in men diagnosed with prostate cancer — which affects about 18,000 Australians according to the Cancer Council.
This means shorter hospital stays and a reduced risk of adverse events during surgery.
An earlier study published in The Lancet in 2016 also found no difference between robotic and open surgery in cancer control, urinary continence and sexual function.

Robotic surgery can make recovery faster. Photo: Getty
These findings provide some comfort for men who face the prospect of choosing between these two types of radical surgery – which can greatly vary in cost.
A report released last year showed the average cost of robotic surgery and hospital stay funded by Medibank in private hospitals varied between $14,553 and $55,928, depending on the surgeon.
The out-of-pocket cost to the patient ranged from 35 per cent in Victoria and up to 88 per cent in NSW and the ACT, according to the Surgical Variance Report, published by the Royal Australasian College of Surgeons and Medibank.
Study author Emeritus Professor Frank Gardiner said that, when it came to choosing the best technique, surgical skill took priority over the type of procedure.
“The most important issues for a good result are an experienced surgeon with good outcome data and somebody with whom the patient can relate comfortably,” he said.
Regarding cancer outcomes, Professor Gardiner said the recent findings should be taken “with circumspection”.
“Two years is but a short time in terms of prostate cancer follow-up,” he said.
What is a prostatectomy?
A radical prostatectomy is a surgical approach to remove the prostate gland and any surrounding tissue that shows signs of cancer.
Traditionally, this operation was done by making a 10-centimetre incision in the lower abdomen. This is called open radical prostatectomy.
Laparoscopic radical prostatectomy is similar, but involves making several smaller incisions through which the surgeon inserts a small camera and instruments to perform the operation.
In robotic-assisted procedures, the specialist uses a computer to remotely control the surgical arm that is inserted through small incisions.

Experts advise gathering as much information as you can before deciding on which procedure to have. Photo: Getty
What do you need to know before choosing surgery type?
For men considering prostate surgery, Professor Gardiner recommends finding out how experienced the surgeon is at performing prostatectomies.
They should also ask about health outcomes and success rates for continence, sexual function and cancer control.
It is also important to have a good rapport with your urologist and build a long-term relationship with them in the post-surgery period.
To avoid unexpected fees, ask for a detailed breakdown of costs when first meeting the specialist and make sure you understand what expenses are covered and which will be out-of-pocket.
The Prostate Cancer Foundation of Australia recommends preparing as many questions as necessary to help you feel at ease before undergoing surgery.
Be sure to understand what the surgery involves, duration, side effects, and how it might affect your sexual function and continence.
You will also need time off work. Recovery times can vary, depending on the technique used and specialists’ advice.
“Recovery time may be quicker with laparoscopic or robotic prostate surgery, compared to open surgery, but all three forms of radical prostatectomy have similar rates of side effects,” a Prostate Cancer Foundation spokesperson said.
“Men should not feel pressured to decide in a hurry. It is also perfectly acceptable to ask for a second opinion.”








