Dodgy doctors to be weeded out under major crackdown
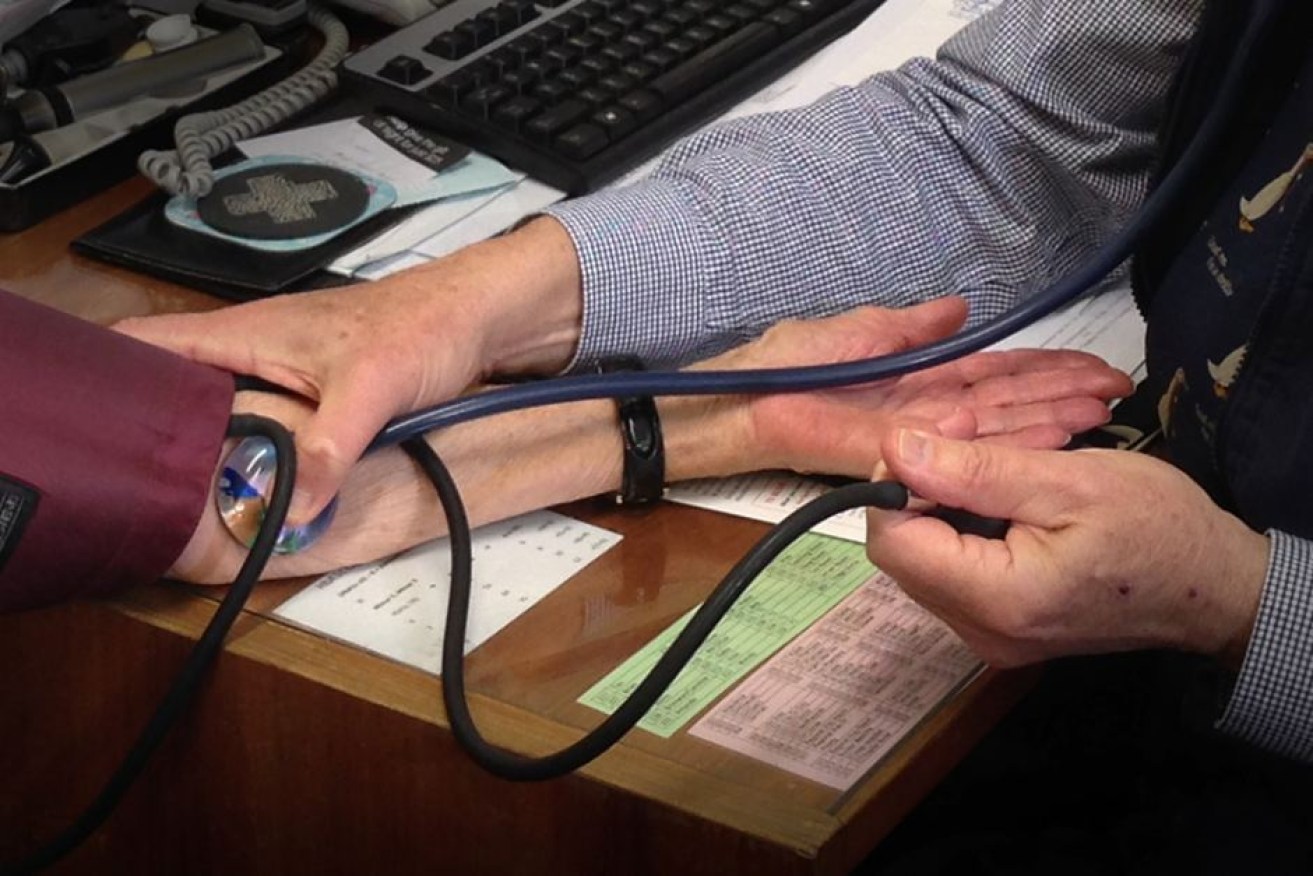
The Medical Board will look more closely at doctors with multiple complaints. Photo: ABC
Health authorities have announced a major crackdown on dangerous doctors to stop them harming patients.
The Medical Board said doctors with multiple proven complaints will have to be assessed by their peers on their performance.
The chair of the Medical Board, Professor Joanna Flynn, said a framework has been developed that will justify and strengthen the trust that the public has in doctors.
“It is focused on patient safety and will support doctors to provide high-quality care throughout their working lives,” she said.
An expert advisory group, set up by the Medical Board, outlined its findings, which have been accepted by authorities.
“It is time for the Medical Board, and other stakeholders in the medical profession, to take steps to proactively identify, assess and manage ‘at risk’ and poorly performing practitioners.”
Research found 3 per cent of Australia’s medical workforce accounts for nearly half of all complaints made to medical regulators or complaints boards.
“This disproportionately high risk of continuing complaints in a very small number of doctors makes clearly evident the pressing need for earlier intervention to prevent the escalation of further complaints and, when relevant, action to protect public safety,” experts said.
Older doctors will come in for extra scrutiny
Medical practitioners aged 70 years will have to undergo a confidential health check, including cognitive screening and a formal managed performance review process.
Research shows those doctors most likely to receive complaints are older, male and those with a history of complaints.
“There is increasing evidence that regular mandatory health checks, including cognitive screening of doctors aged 70 and over, are necessary to protect public safety by identifying and assessing doctors at risk of undetected poor performance,” the expert advisory group said.
“It is possible that a significant number of currently registered medical practitioners aged 70 and over are at risk of poor performance caused by cognitive decline and many more that are experiencing physical decline.”
Practitioners who provide clinical care will have to have peer review and health checks at the age of 70 and every three years after that.
In March 2017, there were 5596 Australian medical practitioners aged 70 years and over and 865 aged 80 years and over, who are registered to practise medicine.
Australian Medical Association (AMA) president Dr Michael Gannon said the AMA acknowledges the need to review medical practitioners who continue to practise over the age of 70.
“As with other professions, it is timely to review a person’s continuing ability to provide care,” he said.
“The AMA will work with the Medical Board and others to develop the health and screening checks for these practitioners.”
But doctors were concerned about proposals to obtain data about individual practitioner’s performance.
“This needs further refinement and we would, in particular, oppose open data sharing between the Medical Defence Organisations and the Medical Board,” he said.
Better training of medical graduates
The expert committee has asked medical schools and specialist colleges to make sure they enforce better standards of behaviour.
“Appropriate professional behaviours should be a mandatory requirement for graduation and for specialist qualifications,” the expert advisory group said.
Research has also shown that risk of complaints is related to poor performance in medical school or speciality training.
“A proven and irremediable lack of professionalism [may] preclude entry to the profession of individuals who are unfit to practise,” the report said.
In addition, medical specialists will no longer be allowed to take part in “self directed” education.
“All doctors will need to complete at least 50 hours of accredited education each year which includes reviewing their performance, outcomes and educational activities,” the report said.
The Medical Board ruled out adopting a controversial system adopted in the UK, where doctors need to re-sit medical exams every five years.
Dr Joanna Flynn said they will be consulting widely with the medical profession on the changes.
“Nothing is going to change tomorrow for individual doctors,” she said.
-ABC








