Toddler reinfused with umbilical blood to stave off diabetes
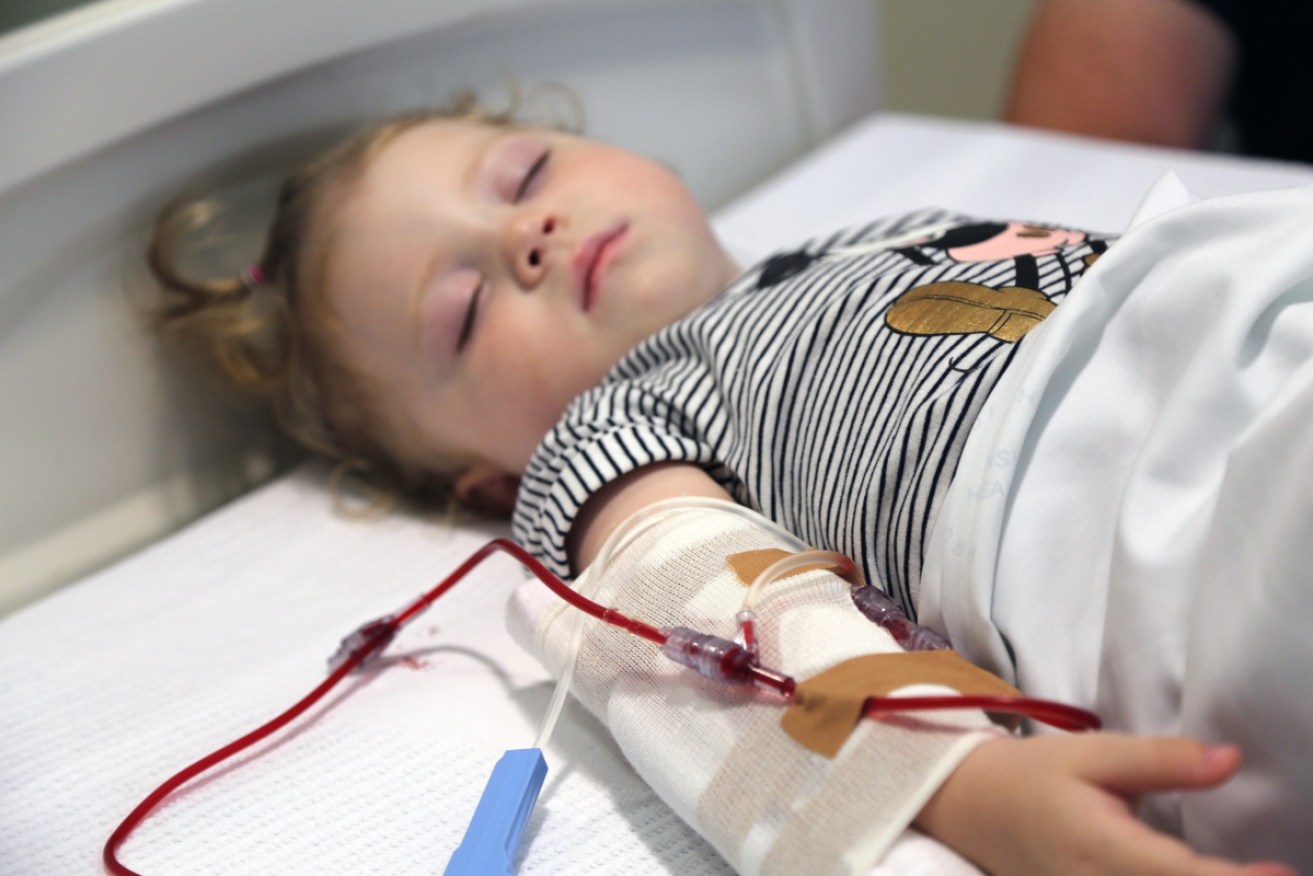
Lucy Hinchion, aged 20 months, undergoing an umbilical cord blood transfusion. Photo: AAP/The Children's Hospital Westmead
A Sydney toddler whose umbilical cord blood was stored to help treat her sister’s Type 1 diabetes has had it reinfused after showing signs of the disease herself.
Lucy Hinchion, aged 20 months, on Friday became the youngest child in the world to receive her own cord blood to help prevent or delay the chronic condition’s onset, as part of a five-year study at The Children’s Hospital in Westmead.
The cells found in umbilical cord blood – unique immune cells called regulatory T-cells, and stem cells – are considered promising in improving the treatment of many diseases including Type 1 diabetes, heart disease, stroke and neurological disorders.

Lucy on Friday became the youngest child in the world to receive her own cord blood to help prevent or delay the onset of type 1 diabetes. Photo: AAP/The Children’s Hospital Westmead
More than 100 Australian children with a family history of Type 1 diabetes are currently being screened in the Cord Reinfusion in Diabetes (CORD) study, conducted through the hospital’s Kids Research Institute and funded by cord blood bank Cell Care Australia.
Sonya Hinchion told AAP her daughter Lucy’s blood has been stored since birth in the hope it would eventually help her seven-year-old sister, Ava, who developed Type 1 diabetes just before she turned four.
Ava’s cord blood was never stored because they have no family history of the disease, Ms Hinchion said.
But after testing positive for two antibodies herself, Lucy became at high risk of developing the condition.
Ms Hinchion said all of Lucy’s frozen cord blood was used in the “textbook” 20-minute procedure last week.
“I think as treatments go, it is one of the easiest and most straightforward things you can do,” she said.
“You’re putting all your eggs in one basket but without doing this trial and without putting yourself out there, we’re never going to learn.
“The other risk is, she develops diabetes and you’ll kick yourself for not trying.”
Approximately 130,000 Australians are living with Type 1 diabetes, with 2000 new cases diagnosed each year.
Ms Hinchion said although Ava deals with her diabetes “beautifully” she has to check her blood glucose level multiple times throughout the day and diligently watch everything she eats.
“You’re putting all your eggs in one basket but without doing this trial and without putting yourself out there, we’re never going to learn.”
Sonya Hinchion
“Diabetes is 24 hours a day, seven days a week,” she said.
She said it was a “no-brainer” to help Lucy avoid diabetes “or at the very least, buy her a few years” and hopes other families will consider storing cord blood.
“It might not be used today or tomorrow but it’s got a long shelf life,” Ms Hinchion said.
“It can be stored for 18-24 years, I think. That’s a long time in science.”
Professor Maria Craig, who leads the study, said ongoing follow-up will occur with Lucy every three to six months for the next three years to monitor her response to the reinfusion.
-AAP








