This harmful disease isn’t being detected or treated
Each year more than 100,000 Australians suffer a fracture due to osteoporosis. Yet leading doctors say very few patients are actually properly diagnosed or treated for the condition, causing their bones to break.
Many will end up back in hospital with more fractures, costing the health system more than a billion dollars.
Only a few Australian hospitals have set up special clinics to ensure patients get the right diagnosis and treatment.
• Forget the dadbod, what about the mumbod?
• Sitting down may increase breast cancer risk
• Why Dr Google is not as dangerous as you think
Professor Markus Seibel runs the fracture liaison service at Sydney’s Concord Hospital and said 70 to 80 per cent of people who go to a GP, hospital or specialist with a bone fracture are not being properly diagnosed and treated for osteoporosis.
Many of those will have subsequent fractures.
“You can imagine for those patients to go through a series of fractures and hospitalisations and operations — it’s devastating not only for them but their families and all of this could’ve been prevented if we intervene early,” he said.

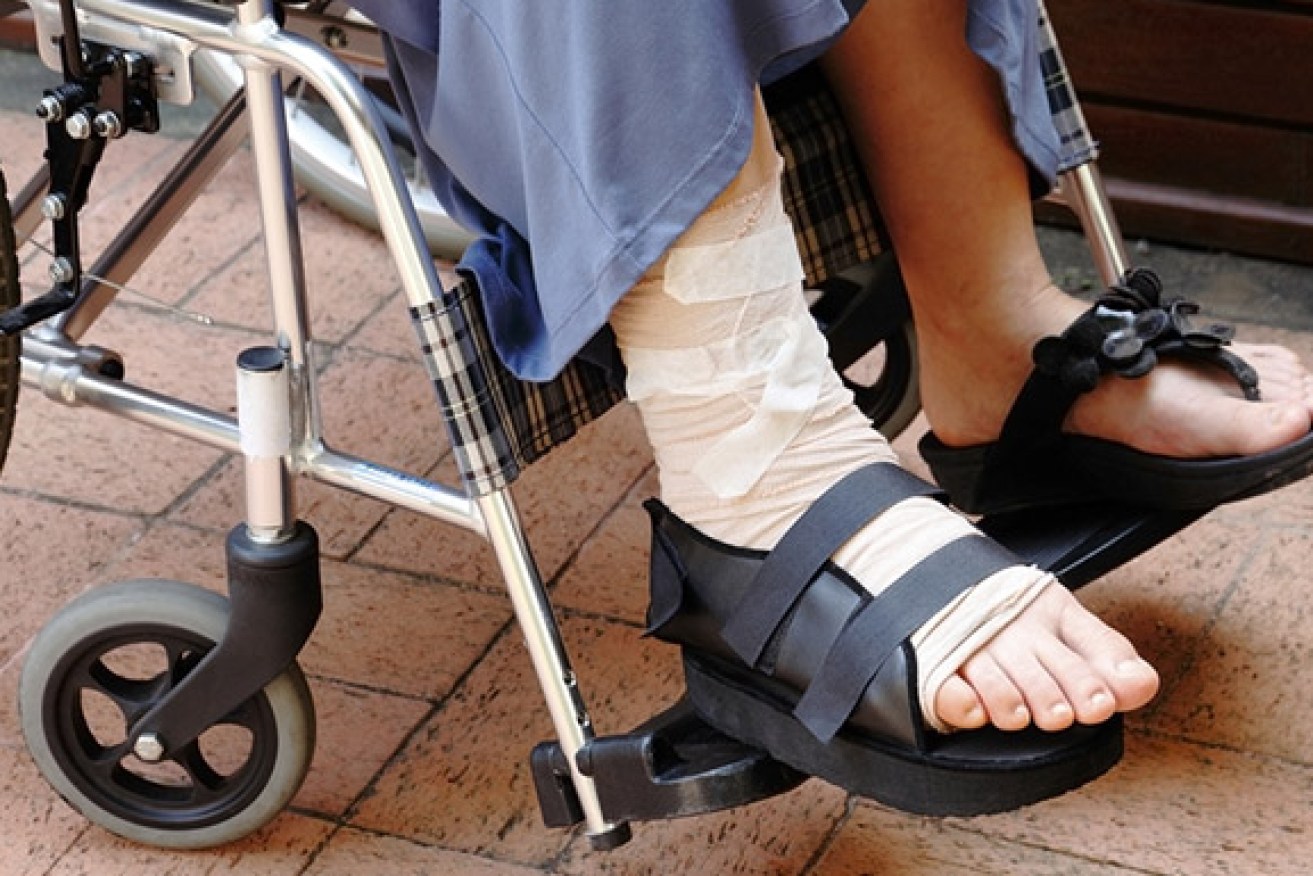
Each year, 140,000 Australians have fractures due to osteoporosis. Photo: Shutterstock
Each year, 140,000 Australians have fractures due to osteoporosis, at a direct annual cost of $1.6 billion.
A group of leading organisations including the Australian and New Zealand Bone and Mineral Society, Osteoporosis Australia and the Royal Australasian College of Physicians are calling for action, to stop the cycle of repeat bone fractures.
“We want a specific action plan with funding mechanisms from state and federal governments to implement secondary fracture prevention programs,” Professor Seibel said.
Bernadette Gallagher, 72, had a number of painful fractures before she was correctly diagnosed with osteoporosis.
“I fell down a pothole and broke my ankle, then both wrists,” she said.
But it was only when she was referred to a fracture liaison service that the cause of her fractures was properly investigated.
“I feel much better having a diagnosis and a treatment plan,” she said.
“Goodness knows how many other Australians are like me walking around with osteoporosis and not knowing it.”
She keeps active, volunteering several days a week at a local hospital and takes mild pain killers to manage the pain.
How is Osteoporosis diagnosed?
Osteoporosis is diagnosed with a bone density scan, commonly known as a bone density test.
It is a simple scan that measures the density of your bones, usually at the hip and spine.
You simply lie flat on a padded table and the arm of the machine passes over your body.
The scan takes approximately 10 to 15 minutes and you remain clothed during the scan.
Your GP will first assess your risk factors for osteoporosis before referring you for a test.
Who should get a scan?
Men and women over 50 with risk factors may need a bone check up with a bone density scan.
If your bone density is low, you are more likely to fracture a bone in the future.
Some risk factors may also require people under 50 to have a bone density scan.
Your bones require calcium, vitamin D and exercise on a regular basis.
Habits like smoking and excessive alcohol intake are bad for bones.
It is also important to be aware of particular risk factors for low bone density.
Risk factors include: family history of osteoporosis, low calcium and vitamin D levels and some conditions or medications.
Source: Osteoporosis Australia
– ABC








