Aussie breakthrough raises hopes of stem cell therapy that lets the body heal itself

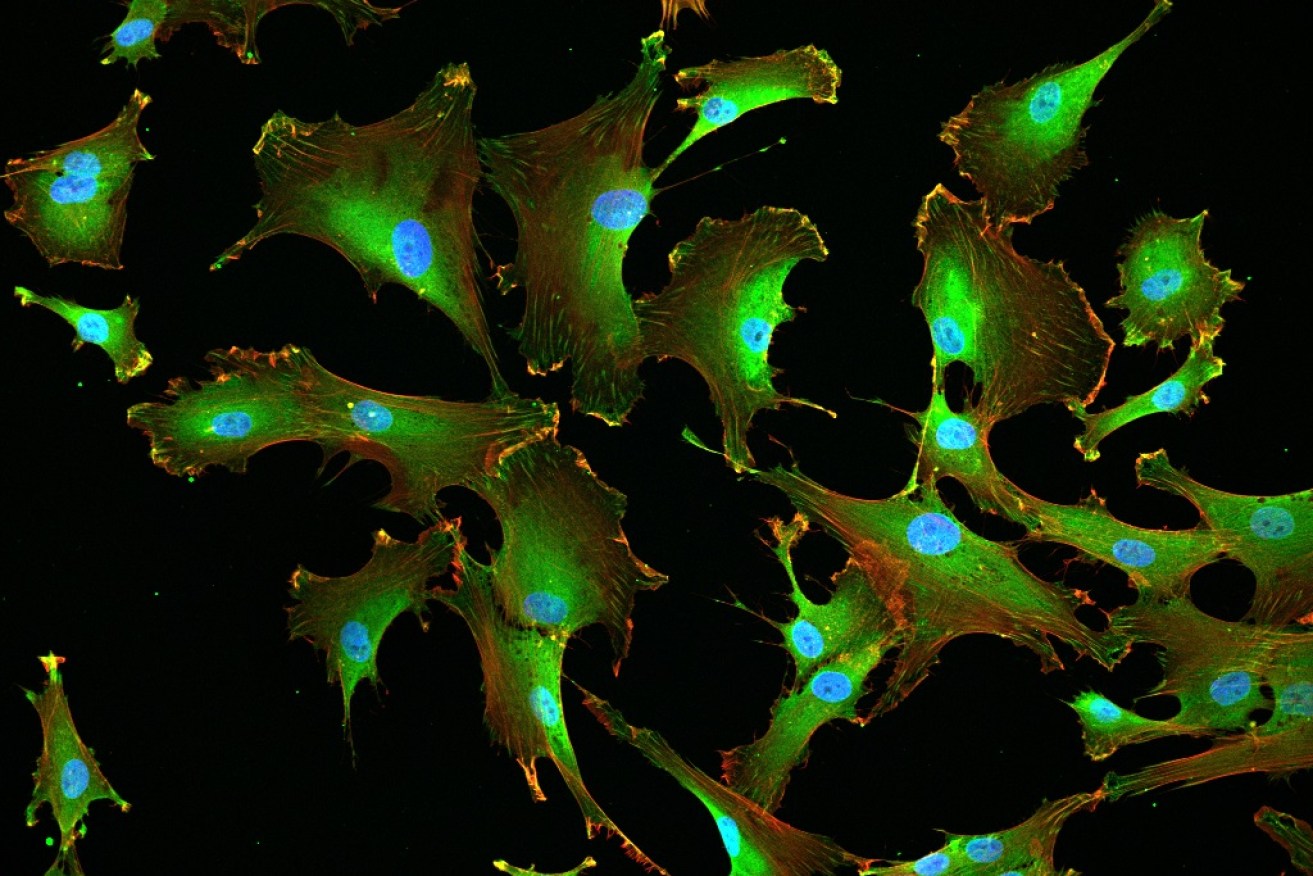
Fluorescently labelled stem cells growing on the tropoelastin protein. Photo: Supplied
A team of international researchers has found a way to grow more vital stem cells cheaply and quickly using a stretchy superglue-like material that was invented in an Australian lab.
If proven successful in human trials the discovery paves the way for a potential new treatment that helps the body heal itself.
Study co-author Professor Anthony Weiss from the University of Sydney’s Charles Perkins Centre collaborated with local and US scientists to develop the technique.
He said the new method facilitated a better environment for stem cells to live and grow.
“Making stems cells requires a process a bit like cooking soup – the more complex the culture or ‘soup’, the more difficult it is to control the growth of the cells and the more expensive it is to make,” he said.
“Our technique simplifies the soup … [and also] encourages other stem cells to join the ‘soup’ – further increasing the rate of growth of the cells.”
Scientists look to nature
For the study, the team relied on an adhesive material called tropoelastin, a versatile and highly flexible molecule that provides the elasticity to our skin, arteries and even our lungs when we breathe.
Dr Giselle Yeo from the University of Sydney, who co-authored the recently published paper, told The New Daily that the team used bacterial cells to make a replica of the human tropoelastin gene molecule in the lab.
“Tropoelastin made using this method is functionally the same as the natural human protein,” she said.
“But it can be made at high quantities and with excellent purity, so it’s really cost-effective.”
The researchers then tested if tropoelastin works in cell growth and repair by applying small amounts of the molecule to human stem cells in a petri dish.
They found that the molecule encouraged more cells to be produced compared to other commonly used proteins for stem cell cultures.
And it’s not the first time, and highly unlikely to be the last, when scientists look to this remarkable molecule for inspiration.
In 2017, Professor Weiss and a US team successfully replicated tropoelastin in the lab, and developed this into a pioneering surgical glue for life-threatening wounds.
The glue, now commercialised under the brand name ‘MeTro’, has the ability to seal wounds shut in 60 seconds without the need for stitches or sutures, making it a powerful tool in medical emergencies such as car accidents or in war zones.

The MeTro glue is squirted directly onto the wound and activated with UV light. Photo: University of Sydney
What’s next?
The researchers expect that, once these stem cells are inside the living body, they will help attract other cells to the the damaged area and kickstart the body to repair itself.
However, human trials are still a fair way off, Dr Yeo said. But the team is hopeful that animal studies will confirm their lab results.
“We want to test the regenerative power of the stem cells we’ve grown with tropoelastin in animals,” she said.
And with the global demand for stem cell technology now overtaking supply, such technologies can help lower the prohibitive cost of cell therapies, Dr Yeo said.
“Stem cells are increasingly being used as cell therapies for a range of diseases that cannot be reliably treated by conventional medicine including skeletal tissue injuries, heart attacks, degenerative diseases and organ failure,” she explained.
“If taken up in commercial cell manufacturing processes, it has the potential to make cell products significantly more accessible.”